Uveitis
What is uveitis?
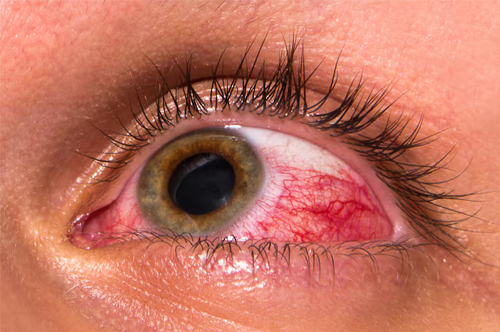
Uveitis is inflammation of the uvea — the middle layer of the eye comprising the iris, ciliary body, and choroid. It can affect one or both eyes and, if untreated, may lead to serious complications including vision loss. Causes include infections, autoimmune conditions, systemic diseases, or may be idiopathic (no identifiable cause).
What are the symptoms of uveitis?
Symptoms may include eye redness, pain, sensitivity to light (photophobia), blurred vision, and floaters. In some forms — particularly in children — uveitis can be entirely asymptomatic, making regular screening essential.
How is uveitis treated?
Treatment depends on the underlying cause and severity. It may include corticosteroid eye drops, periocular or intravitreal injections, oral corticosteroids, immunosuppressive agents (such as methotrexate), or biologic therapies (such as adalimumab or infliximab). A joint approach involving the ophthalmologist and rheumatologist is often required for systemic disease.
Can immunosuppressive medications be used in uveitis?
Yes, in cases where corticosteroids alone are insufficient or cause unacceptable side effects. Methotrexate is now considered a first-line corticosteroid-sparing agent. The choice of immunosuppressive therapy is made jointly by the ophthalmologist and rheumatologist based on the individual patient's disease profile and overall health.
Can biologic therapies be used in uveitis?
Yes. In cases refractory to conventional immunosuppressives, biologic agents targeting specific inflammatory pathways are increasingly used. TNF-α inhibitors such as adalimumab and infliximab are commonly employed. Agents such as tocilizumab and abatacept are considered in more refractory cases. All biologic treatment is tailored to the individual patient.
What is paediatric uveitis?
Paediatric uveitis refers to uveitis occurring in children. It accounts for 5–10% of all uveitis cases. It differs significantly from adult uveitis in that it is frequently asymptomatic, tends to follow a chronic course, and carries a higher risk of complications such as cataracts, glaucoma, and band keratopathy. Diagnosis is often delayed due to the difficulty of performing a comprehensive eye examination in young or preverbal children.
How common is uveitis in children, and is it more serious than in adults?
While less common than adult uveitis, paediatric uveitis tends to be more severe. A higher proportion of children present with posterior uveitis (40% in children versus 20% in adults), and the smouldering, asymptomatic nature of the disease in children makes early detection and close monitoring particularly important.
Do children outgrow uveitis?
? In some conditions, particularly JIA-associated uveitis, the inflammation may gradually resolve over time. However, reaching this stage without complications or vision loss is extremely challenging and requires diligent, long-term management. Regular follow-up must be maintained even when the child appears symptom-free.