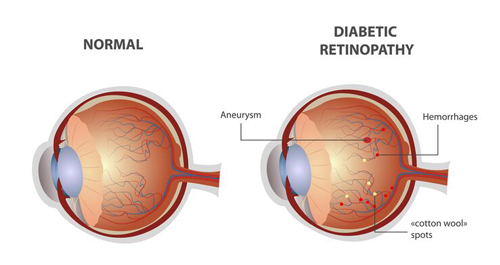
Diabetic Eye Disease
How do I know if diabetes is affecting my eyes?
Diabetic eye disease can be asymptomatic in its early stages, which is why annual comprehensive eye examinations are strongly recommended for all patients with diabetes — even in the absence of symptoms. When symptoms do occur, they may include blurring of vision, floaters, or sudden loss of vision.
Why does my vision become blurred with diabetes?
Rapid fluctuations in blood sugar levels can cause fluid shifts in the lens, temporarily altering its shape and affecting focus. This blurring typically resolves when blood sugar stabilises. However, prolonged or severe changes in blood sugar can cause the lens to swell and may contribute to cataract formation.
Can diabetic retinopathy be reversed?
Damage already caused by diabetic retinopathy is generally permanent. However, early and sustained blood sugar control can slow progression and, in some specific cases, lead to partial improvement. Most treatments aim to prevent further vision loss rather than restore lost vision. Early detection is therefore critical. Your doctor will help you understand the treatment options most appropriate for your stage of disease.
Can I drive with diabetic retinopathy?
In the early stages of the condition, driving may remain possible. Your ophthalmologist will assess your visual function at each visit and advise you accordingly — including any restrictions on night driving or whether driving should be avoided altogether.
How can I slow the progression of diabetic retinopathy?
Maintaining well-controlled blood sugar, blood pressure, and cholesterol levels is the most effective strategy. This involves a combination of healthy lifestyle choices, appropriate medication, and regular monitoring in coordination with your physician and ophthalmologist.
How many anti-VEGF injections will I need?
The number and frequency of anti-VEGF injections depends on the severity of retinal swelling, the specific medication used, and your individual response to treatment. Injections are typically administered every four to six weeks initially, followed by a tapering schedule. Your ophthalmologist will personalise your treatment plan and revise it based on your response.
Is laser treatment for diabetic retinopathy painful?
Laser photocoagulation is generally well tolerated. Patients may experience a mild stinging sensation or brief flashes of light during the procedure. Anaesthetic eye drops are used beforehand to minimise discomfort.
What investigations are done for diabetic retinopathy?
A comprehensive dilated fundus examination is the primary diagnostic tool. Additional investigations may include:
- OCT (Optical Coherence Tomography) — to detect and quantify retinal swelling
- FFA (Fundus Fluorescein Angiography) — — to identify leaking blood vessels and areas of non-perfusion
Diagnostic Tests: OCT & FFA
What is an OCT (Optical Coherence Tomography) scan?
OCT is a non-invasive imaging technique that produces cross-sectional images of the retina — similar in concept to a tissue biopsy but without any contact or discomfort. It can detect fluid accumulation, structural damage, and early signs of conditions such as diabetic retinopathy, macular degeneration, and glaucoma.
How is an OCT performed?
The patient sits comfortably, rests their chin on a chin rest, and focuses on a target light. The OCT machine scans the eye without touching it. The procedure is painless and takes only a few minutes.
What conditions can OCT help diagnose?
OCT is used in the evaluation of: macular hole, macular pucker, macular oedema, age-related macular degeneration (AMD), glaucoma, central serous retinopathy, diabetic retinopathy, and vitreoretinal traction.
What is FFA (Fundus Fluorescein Angiography)?
FFA is a diagnostic procedure in which a water-soluble fluorescent dye is injected into a vein in the arm. As the dye circulates through the retinal blood vessels, a series of photographs is taken using a specialised fundus camera. It helps identify leaking vessels, areas of poor blood supply, and structural abnormalities in the retina.
Is FFA painful? Is it safe?
There may be a brief, mild discomfort when the cannula is inserted. The imaging itself is entirely painless. The procedure is generally safe and performed with all standard precautions. Some patients may notice a temporary yellowish tinge to their skin and brighter-coloured urine for up to 24 hours — both are harmless and resolve on their own.
Can I drive home after an FFA test?
We advise patients not to drive until the effect of the dilating (mydriatic) eye drops has worn off. This can take up to six hours, and in some cases may persist until the following day. Please arrange for someone to accompany you or plan alternative transport.